Welcome to FALLARREST.com – the home of fall protection!
This platform, and our associated developed platforms have been designed primarily to provide important information relating to working at height, fall prevention & protection, however, the platform also lists our partners & solutions for working at height. We have made this as simple as possible for you so that you can cherry-pick the information that you require.
Please use the navigation menu on the left of our page (or if on mobile the icon in the top right of the screen) for information regarding the fall protection solutions that we can offer.
Our vision and mission have been to develop various resources to provide advice, information, and solutions for working at height to make it easier for people to understand the dangers of working at height and our solutions. You can find them below;
harnesses.com – this is our online platform for harnesses, lanyards, hard hats, scaffolder kits, MEWP kits, and other associated personal protective equipment.
We registered and developed the site into an online e-commerce web platform to run adjacent to our fall protection businesses, this enables us to be able to provide high-quality personal protective equipment at unbeatable costs, in some cases, you will find 25-50% savings on the same product that other providers sell for, making PPE affordable for more people, hence improving safety.
rooflightcovers.com – with the rise in solar panels being installed, and with thousands of buildings being 25-30 years old, PV contractors & clients are finding it extremely challenging to be able to install the solar on the roof safely, and to undertake the required continued maintenance works.
We work with our PV partners to provide safe access for the installation works, as well as protection for the maintenance of the systems for the next 25+ years! Fragile roof lights are a huge concern, and very high risk, we provide a choice of various types of cover.
standingseam.com – is a roofing material. It is designed to have no penetrations. This platform provides information and solutions for working at height when working with/on standingseam.
freestandinghandrails.com – this is a selection of the types of handrails that we can provide.
Cable-based fall protection, modular skylight protection, eyebolts, fixed eyebolts, removable eyebolts, ladders, caged and fixed access ladders, companionway ladders, roof walkways (plastic, aluminum, non-slip, galvanised, GRP), steps, platforms & gantries, stepover platforms, access gantry platforms, facade access, davit arms & sockets, abseiling anchors, lightning protection, roof surveys, provision and sale of personal protective equipment, annual recertification & testing, health and safety training, guttering services, access hatches, onsite welding, roof lights, hire equipment, PV panels/solar energy, roofing membranes, liquid plastics, demarcation zoning, and further services on request.
Fallarrest.com is one of the longest-standing and original fall protection providers in the UK. After having 25 years of experience within this industry, we have forgotten what most know! We have designed & installed systems for famous landmarks, as well as famous people’s houses, from low-value projects to over £500k.
We are a reputable and honest company placing a high emphasis on service, morals, and integrity. We are not concerned about the value of a project, or the vanity of turnover, we are in the business of keeping people safe!
Our vision is to create a platform that offers complete envelope roofing solutions including information and provision for associated personal protective equipment that is commonly used with fall protection systems. We are uniquely placed to be able to facilitate all of your requirements on one platform. This will save you time trawling through multiple websites, manufacturers, and installers for information relating to all roof-associated products from a trusted source.
We can assist in the design, supply, installation, and recertification of fall protection equipment as well as the supply of personal protective equipment (PPE) via our sister platform harnesses.com where we are uniquely placed to offer advice and supply of leading, innovative and highly engineered products ranging from harnesses, lanyards, personal rescue devices, SRL units, mini SRL blocks, rescue kits, free standing non-penetrative weighted anchors and much more for use in conjunction with fall protection systems.
There are many choices of fall protection systems within the marketplace, some that may not work, and a vast number of companies that lack the training & understanding of fall protection. In recent years there has been a vast number of companies that have ‘sprung up’ seeking profits over safety as well as labour supply companies that supply untrained and unskilled labour to the industry.
We are extremely proud to be associated on our page with leading recognised and reputable names in the industry, a testament to the trust that is instilled in us and we would like to thank them for being part of our vision.
Fallarrest.com operates on a global platform, therefore we are well placed to assist you regardless of your geographical location.
All of the products listed on this site are generally available through an approved distributor network only. Fallarrest.com are approved to supply and install for all of the manufacturers listed, however, we have provided the links to our partner websites for ease of navigation as in all instances there is an enormous amount of further high quality and engineered products that can be found on their websites. Please do not hesitate to contact us as we can put you in touch with the right people and the service or product that you are looking for.
Falls from height remain one of the most common causes of injury and fatality at work accounting for nearly 30% of injuries to workers. It is a stark reality that in an age where working at height is commonplace that fall protection measures still need to be much more effective.
According to fall protection manufacturers, a three-pronged approach to fall protection is required. Namely engineering innovation, compliance, regulations, and representative test methods.
‘Scaffolds, handrails, barriers, and movable platforms can be constructed to protect workers employed at heights. Where these devices are impractical, personal fall protection equipment such as full-body harnesses, lanyards, and retractable lifelines may be used.’
Fall protection can create a minefield of complexities and hazards and should only be carried out by trained, competent, and authorised people. We hope that our web site will provide you with guidance on what you need to know, what to do and how to do it.
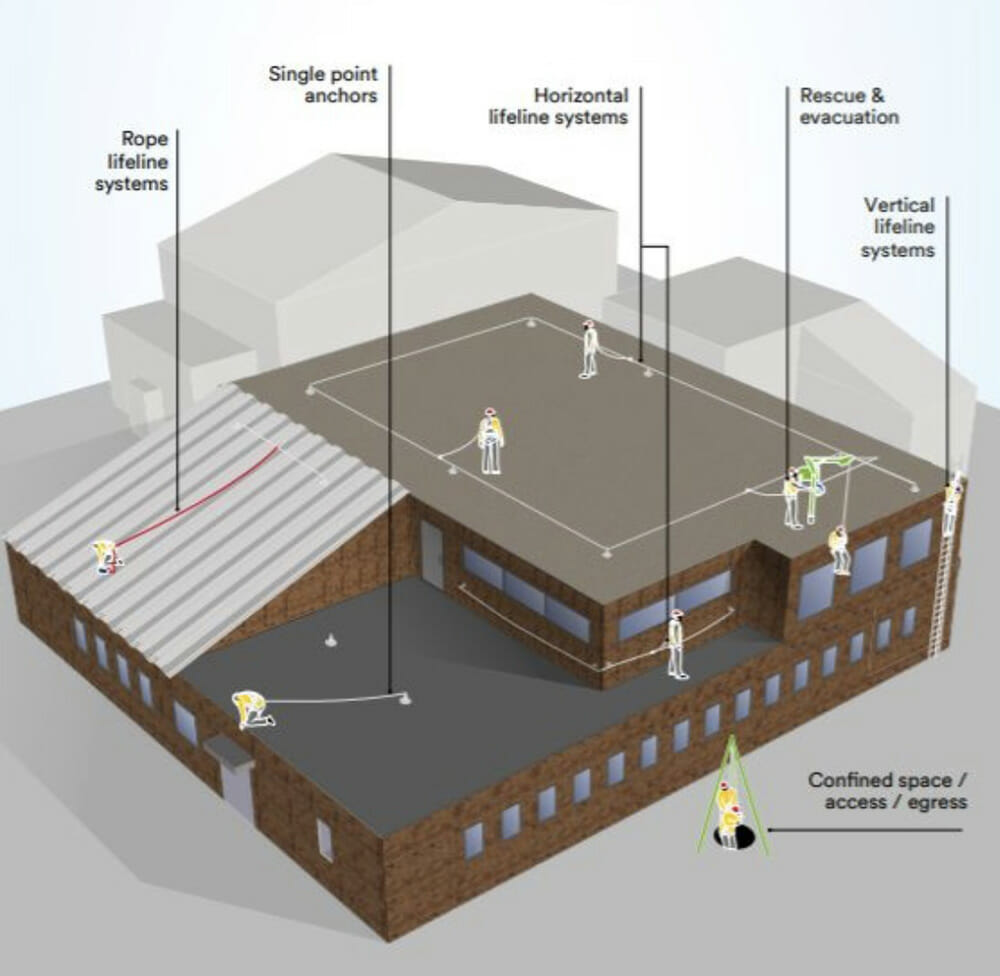
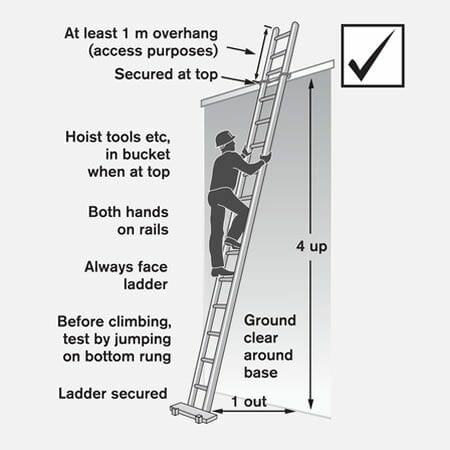
Please use the menu for further information appertaining to each section.
Fall arrest is the term used for when somebody ‘falls from height’ and their fall is ‘arrested’.
Fall restraint is the term used for when somebody is restricted from reaching the fall hazard, thus restrained.
Testing & recertification is the term used for when a fall protection system must be tested at intervals no greater than 12 months as per legislation.
Harnesses are what is required as part of the personal protective equipment (PPE) to be worn when using a fall protection system.
Access Ladder is a means of access and egress to a roof.
We will explain the fall protection market, what is fall protection, falls from height, the difference between fall arrest and fall restraint, what you should consider when designing fall protection, window cleaning at height, the risks and dangers of suspension trauma, legal requirements around the world and the importance of annual testing and recertification of installed fall protection systems.
We hope that you find the site informative and interesting. However, should you have any questions or require any additional advice, please do not hesitate to contact our team via our contact form or email info@fallarrest.com





